This is the first of several reviews on the treatment of Attention-Deficit/Hyperactivity Disorder (ADHD), with a focus on children and adolescents. In the next review, we will focus on the evidence-based treatments of ADHD in adults.
In today’s Wassup’ review, we evaluated a 2017 meta-analysis examining the evidence-based treatments for children and adolescences with ADHD.
In the current systematic review and meta-analysis, the authors evaluated a total of 190 randomised controlled trial studies involving 26,114 participants assigned to either treatment or control conditions. The participants were aged between 3 to 16 years old and were predominantly male (77%; 23% females).
Various treatments for ADHD were evaluated against a control. They were:
- Pharmacotherapy:
- Stimulant medication
- Non-stimulant medication
- Antidepressants
- Antipsychotics
- Other unlicensed drugs (drugs not approved for use in ADHD)
- Psychological interventions:
- (Cognitive) Behaviour therapy
- Cognitive training (e.g. attention training)
- Neurofeedback
- Complementary and alternative medicine (CAM) interventions:
- Dietary therapy (e.g. restricting diet)
- Polyunsaturated fatty acids (e.g. omega-3 fatty acids)
- Vitamins & Minerals (e.g. vitamin B6, magnesium, zinc, calcium)
- Amino acids (e.g. glycine, L-tyrosine)
- Herbal therapy (e.g. ginkgo, ginseng)
- Homeopathy
- Others
To determine the effectiveness of treatment, participants were evaluated using standardized tools measuring their global functioning or ADHD symptom severity. Participants were considered as having made improvements if they were rated as ‘much improved’ or ‘very much improved’ on their global functioning, or had a reduction of at least 25% on an ADHD symptom severity rating scale.
Effective Treatments
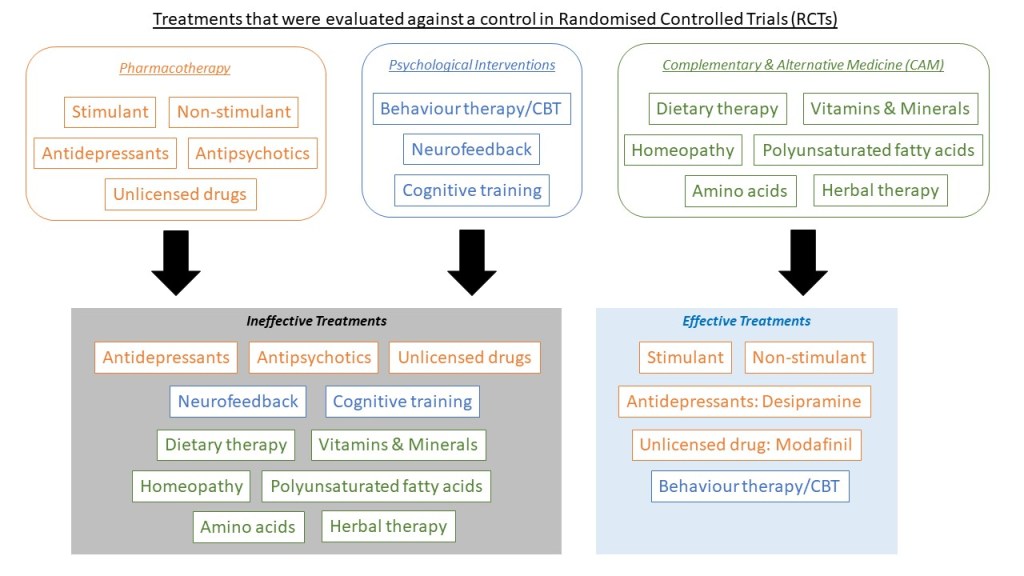
From the network meta-analysis, there were some low-quality evidence that behaviour therapy/CBT, stimulant medication, or non-stimulant medication were superior to placebo/control in the treatment of children and adolescents with ADHD.
A closer examination of pharmacotherapy revealed that the following medications were more efficacious compared to a placebo:
- Methylphenidate (stimulant),
- Amphetamine (stimulant),
- Atomoxetine (non-stimulant),
- Guanfacine (non-stimulant),
- Clonidine (non-stimulant),
- Desipramine (antidepressant), and
- Modafinil (an unlicensed drug)
For behavioural therapy/CBT, a combination of child, parent and/or teacher training was more effective than controls in the treatment of ADHD in children and adolescents.
There was also evidence that combination treatments were effective in treating ADHD in children and adolescents. Specifically:
- Stimulants + behaviour therapy
- Stimulants + non-stimulants
- Non-stimulants + behaviour therapy
- Stimulants + antipsychotics + behaviour therapy
- Stimulants + antipsychotics
- Stimulants + other psychotherapies
- Stimulants + polyunsaturated fatty acids
- Stimulants + minerals
- Stimulants + herbal therapy
However, it should be noted that when evaluating combination treatments, some of the observed effects could be attributed to the presence of stimulants, non-stimulants, or behaviour therapy effects.
Treatments with no evidence of effectiveness
The following treatments were found to be ineffective in the treatment of ADHD in children and adolescents:
- Cognitive training
- Neurofeedback
- Antipsychotics
- CAM interventions (e.g. dietary therapy, polyunsaturated fatty acids, minerals, herbal therapy, homeopathy)
It should be noted that while the above treatments were found to be ineffective at the time of the review, more evidence may emerge in future that challenge the status. For example, there is some low quality but emerging evidence that mindfulness-based intervention may be effective in treating ADHD and inattention.
Side effects of treatment
While pharmacotherapy (with or without behaviour therapy) may appear to be the treatment of choice for ADHD, we should also be cognizant of the associated risks in the form of side effects.
From the meta-analysis, the following side effects were reported by participants:
- Anorexia
- Weight loss
- Unspecified sleep disturbances
- Insomnia
- Anxiety
- Serious adverse events

Conclusion
ADHD is a neurodevelopmental condition that affects between 3-7% of young people globally. As it stands, pharmacotherapy in the form of stimulant and non-stimulant medicine, as well as behavioural therapy/CBT appear to be the dominant forms of intervention with demonstrated effectiveness in managing the condition in children and adolescents aged between 3 and 16 years old. A combination of stimulant medication with behaviour therapy/CBT might be a suitable regime. This is consistent with the recommended guidelines by the National Institute for Health and Care Excellence (NICE) UK. While pharmacotherapy is widely considered by many individuals and parents, we should also be aware of the possible side effects that occur. Finally, it should be noted that the strength of evidence for the above is mostly low quality. More high-quality studies are required to validate the current treatment regimes, as well as to determine if there may be alternative forms of treatments that individuals with ADHD may also benefit from.
Eugene


2 thoughts on “Research Review: Evidence-based treatments for children and adolescents with ADHD”